In 2026, the healthcare industry finds itself at a crossroads. After decades of prioritizing efficiency, volume, and late‑stage intervention, the system is confronting a stark reality: the dominant drivers of illness emerge years before traditional care ever intervenes. Despite unprecedented spending, nearly $5 trillion annually in the United States, the vast majority of that investment goes toward treating chronic disease and managing symptoms after they appear.
Meanwhile, preventive opportunities go largely unclaimed. In the midst of this reckoning, signals an important shift in how care can be organized, measured, and delivered. Longevitix argues that healthcare needs its own “food pyramid moment,” a foundational framework that reflects human biology rather than industrial incentives.
The Healthcare System’s Structural Challenge
Modern healthcare resembles the food systems that prioritize industrial efficiency over biological reality. For decades, broad dietary pyramids and government nutrition advice endorsed high intake of industrialized, processed foods, a pattern that has contributed to poor metabolic health outcomes: ultra‑processed foods now comprise nearly 62 % of calories among American youth and more than half of adult caloric intake. This metabolic imbalance is not only a dietary concern. It is emblematic of a system designed for reactive problem-solving, rather than sustained predictive health maintenance.
Chronic diseases rooted in metabolic dysregulation, inflammation, and lifestyle factors now dominate the public health burden. Despite well‑validated preventive guidelines, their real‑world uptake is limited. Only about 8 % of U.S. adults aged 35 + receive all recommended preventive services, while nearly 5 % receive none. These figures underscore that the current care infrastructure is misaligned with early health trajectories and long‑term wellness goals.
Why Continuous Biological Insight Matters
One of the most promising shifts underway lies in how health data is generated and applied. Traditional care captures health snapshots, annual check‑ups, intermittent labs, and episodic visits, which offer only a partial view of a living system. By contrast, digital biomarkers collected via wearables, smartphones, and remote sensors provide continuous, real‑world physiological data that can reveal subtle shifts before they escalate into chronic disease.
Recent research highlights the value of digital biomarkers in capturing patterns of fatigue, activity, sleep, and autonomic function across a range of chronic conditions, offering a richer view of disease progression than static tests alone. Passive monitoring of heart rate variability, movement, and sleep efficiency, signals once accessible only in clinical settings, can now be tracked non‑invasively and continually through wearable technology.
These continuous data streams, when coupled with advanced analytics, support early risk detection and personalized interventions, the very elements missing from traditional episodic care models.
Longevitix’s Healthcare Pyramid: Inverting the Hierarchy of Care
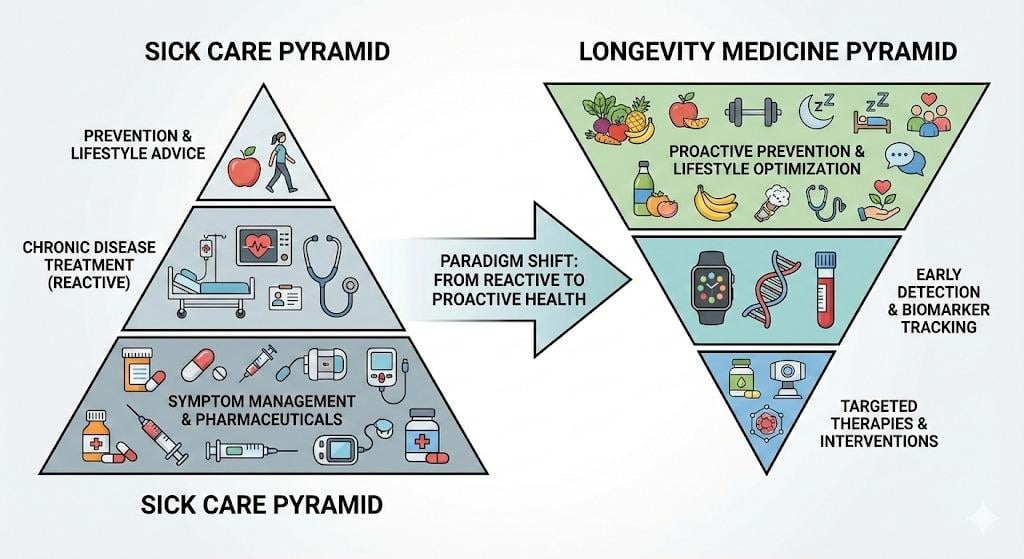
At the heart of Longevitix’s vision is a redesigned clinical hierarchy that acknowledges where value truly lies in modern care delivery. Its Healthcare Pyramid presents an inverted model that places prevention and biological insight at the base, rather than at the periphery:
- Foundation: Proactive Prevention & Lifestyle Optimization — Rooted in personalized biology rather than generic clinical guidelines, this level emphasizes long‑term health behaviors, nutrition, metabolic balance, and environmental factors.
- Middle Tier: Continuous Monitoring & Early Detection — Enabled by digital biomarkers, wearables, and molecular diagnostics, this tier focuses on capturing early physiological deviations long before they escalate to clinical thresholds.
- Apex: Targeted Therapies & Precise Interventions — Treatments, medications, and clinical procedures are reserved for times when they are objectively needed, informed by longitudinal data rather than reactive responses to symptomatic disease.
This inverted pyramid does more than rearrange conceptual priorities; it realigns incentives and decision‑making toward maintaining health rather than managing decline.
Rebalancing Incentives and Outcomes
Both healthcare and food systems face a shared structural dilemma: incentives that favor short‑term efficiency and volume over long‑term biological resilience. In nutrition, this has meant subsidies and guidance that historically under‑weighted metabolic health. In clinical care, this has meant reimbursement structures and care delivery models that reward procedural interventions over sustained, personalized monitoring and preventive action.
Emerging evidence indicates that upstream investments in prevention, particularly those grounded in early risk detection through continuous monitoring, can yield both better health outcomes and long‑term cost savings. Digital health interventions show promise in improving chronic disease self‑management, with continuous data helping clinicians and patients stay engaged and responsive to evolving health signals.
Longevitix’s Healthcare Pyramid embeds this logic into a practical framework, supporting a broader shift from reactive sickness care to proactive healthspan management.
Evolving Care Around Biological Truths
Healthcare’s historical blind spot has been its episodic nature: clinicians reacting to what has already gone wrong rather than anticipating what could go wrong. By inverting the traditional care pyramid, Longevitix offers a compelling counter‑narrative, one that places continuous biological insight at the center of decision‑making and preventive action well before illness takes shape.
The Healthcare Pyramid isn’t merely a visual redesign; it is a philosophical recalibration that positions healthspan, the period of life lived in good health, as the organizing principle of modern care. In doing so, Longevitix’s framework charts a path toward a future where healthcare begins long before diagnosis, guided by the rhythms of biology rather than the urgencies of crisis.


